- NLI Research Institute >
- The Introduction of Market Mechanisms for Long-term Care Services - An International Comparison with Implications for Japan -
The Introduction of Market Mechanisms for Long-term Care Services - An International Comparison with Implications for Japan -
Kazuhisa Go
Font size
- S
- M
- L
| 1. The Global Trend Toward Market Mechanisms
There has been a global trend toward introducing market mechanisms for social services such as education, social insurance, and medicine, and long-term care services have been no exception. Since the 1980s, long-term care services in the West (Europe, the U.S., and Australia) have been increasingly exposed to market mechanisms, causing the supply of services to shift gradually from the public sector to the private sector. The following table illustrates this trend in the West from the viewpoint of policies to promote a mixture between public and private sectors in supplying long-term services.
|

| (1) U.S.
Since the Reagan administration came to office in 1981, the at-home care industry has grown rapidly due to the expanded coverage of Medicare and Medicaid and deregulation of at-home care for the elderly. Growth in the care services industry has been strong; from 1986 to 1995, revenue growth of companies that manage long-term convalescent facilities has averaged 9.5 percent annually, while that of at-home care and at-home medical service providers has averaged 19.6 percent over the same period.1 (2) U.K. Traditionally, long-term care services in the U.K. had been in the public domain. But since the Community Care reform in 1992, public agencies have been required to compare the cost-effectiveness of providing services themselves and outsourcing to private firms (a separation of supply and purchasing functions). As a result, many operations have been reduced or eliminated by a growing reliance on outsourcing and subsidies to the private sector. Looking at the number of elderly homes between 1984 and 1994, while privately run facilities grew an average of 9.9 percent annually, those run by private non-profit organizations grew only 2.6 percent, and public facilities actually contracted by 5.5 percent annually.2Thus the U.K. has transformed its welfar e system from a cradle-to- grave welfare state to a quasi-market multi-dimensional welfare system emphasizing the private sector. (3) Germany In the past, six major non-profit welfare organizations including Deutscher Caritasverand and the Red Cross had received public funding to supply long-term care services. The services they provided, which enjoyed prestige as public services and accounted for approximately 50 percent of all such services, constituted a barrier to entry for private companies. However, since the introduction of long-term care (LTC) insurance in 1995, the competitive conditions between welfare organizations and private companies have become more equal due to measures such as reduced subsidies to welfare organizations and expanded subsidies to private companies for construction. In addition, small unknown private service providers are finding the contracts with Pflegekas sen (long-term care insurers) useful both in gaining vital user in formation and gaining the trust of users. Thus the long-term care insurance system is playing a critical role in introducing market mechanisms. (4) Australia Traditionally, private welfare organizations have been responsible for elderly welfare, with the government providing funding. Private companies were already allowed to run nursing homes when in 1991 the Aged Care Reform Strategy further allowed private companies to operate hostels (residential facilities for elderly persons who do not need constant nursing care but have difficulty living at home). In response to the sharp increase in at-home care demand triggered by reforms (specifically the Home and Community Care Act of 1985), many personnel-supply agencies have been established to provide home helpers. (5) Sweden Sweden is known as a welfare state financed by one of the highest tax rates in the world, and the majority of long-term care services have been supplied by the public sector. However, since the Ädelreforms in 1992, the private sector has gradually begun playing a role, primarily in the form of subcontracting long-term care facilities, at-home care services, meal services, and transportation services in urban areas such as Stockholm, Gothenburg, and Malmö. The ratio of private sector subcontracting (value basis) has risen from 1 percent in 1991 to 4 percent in 1995. As a result, large multinational companies have emerged such as Stockholm-based Partena who specialize in businesses subcontracted by the public sector.
2. Background to the Introduction of Market Mechanisms The following factors are considered to have encouraged the introduction of market mechanisms in the once predominantly public-sector domain of long-term care services. (1) Rising Social Security Costs In Europe, the reduction of fiscal deficits has been a high priority among prospective member nations ahead of the scheduled start of the EMU in 1999. To reduce rising social security costs, governments are pursuing efficiency in welfare operations by introducing competition and shifting to private providers. (2) Transfer of Authority to Municipalities Since the 1980s, due mainly to a growing emphasis on local decision-making in social welfare matters, municipalities have been delegated greater authority, accountability, and financial power in administering social welfare (the Community Care reform in the U.K. and Ädelreforms in Sweden are representative examples). Financial responsibility has led local authorities to develop greater cost awareness and adopt outsourcing alternatives when the availability of experience, human resources, and expertise is in question. This decentralization of welfare has encouraged the shift to private providers. (3) Shift to At-home Care The 1980s saw a substantial shift in the West from institutional care to non-institutional, at-home care. Since at-home care had lagged behind institutional care in developing systematic welfare services, the shift to at-home care opened up new opportunities for the private sector. These three factors formed the backdrop to the elderly welfare reforms implemented in various countries from the late 1980-the Community Care reform in the U.K. (from 1992), Ädelreforms in Sweden (from 1992), Aged Care Reform Strategy in Australia (from 1985), and nursing home reform in the U.S. (late 1980s to early 1990s). All of these reforms were aimed at achieving a more efficient supply of services and containing costs, and as a result promoted a shift in supply to the more productive private sector. While the introduction of long-term care insurance in Germany differs in timing and content from the other reforms, it shares with them the effect of introducing market mechanisms.
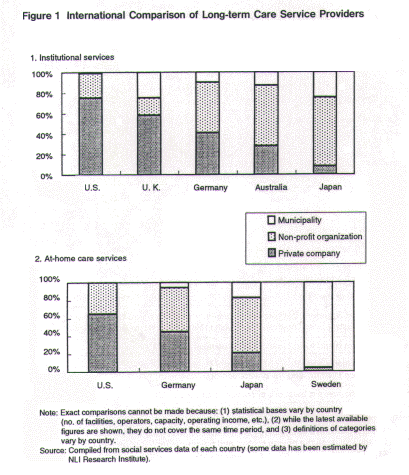
3. U.K. and U.S. Lead the Shift to Private Providers3 As a result of introducing market mechanisms to long-term care services in the West, the proportion of long-term care services supplied by private providers has surged in the past decade. However, much of the private sector participation in Europe (excluding the U.K.) consists of non-profit organizations, while for-profit private companies remain a minority. Leading the shift to private providers are the U.S. and U.K. While public long-term care services technically exist in the U.S., the quantity and variety of services are extremely limited.4In the U.S., most long-term care services are supplied by private companies and non-profit organizations. There are many large health care companies including at-home care service providers such as Kelly, Olsten, and Caretenders Health Corp. (the first two companies are entries from the personnel agency industry), and nursing-care facility operators such as Beverly Enterprises and Sun Healthcare. In the U.K. as well, following the Community Care Reform, the private sector's market share has risen wit h the emergence of nursing-care facility operators su ch as TC Group (Care First), Care U.K., and ANS. In between these two extremes are Germany, Australia, and Japan, where the public and private sectors coexist while complementing and competing against each other.
|
|
4. Japan in Comparison to the West In Japan, long-term care services can be classified into public welfare services provided by municipalities, Shakai Fukushi Hojin(social welfare corporations), and Shakai Fukushi Kyogikai(Councils of Social Welfare) on the one hand, and "silver services" provided by the private sector on the other.5While the public and non-profit sector's role is overwhelming at present, the private sector has been steadily expanding its role in recent years. For example, the private sector's at-home care market grew 22.8 percent annually from 1990 to 1993.6 |
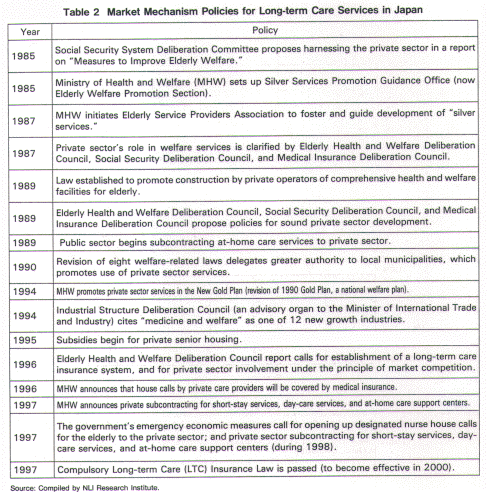
| Japan shares much with the West regarding the background factors that promote market mechanisms. First, social security costs are also rising in Japan. Second, the decentralization of welfare administration was promoted by the 1990 revision of eight welfare-related laws, which enables municipalities to operate elderly welfare services on their own. Moreover, when municipalities become insurers under the new LTC insurance system, their responsibilities will increase further. Third, regarding the shift to at-home care, Japan began building a substantive framework for at-home welfare in the 1990s with the Gold Plan (the Ministry of Health and Welfare's welfare plan formulated in 1990). Fourth, as in Germany, the introduction of LTC insurance (in April 2000) is certain to mark an epoch in elderly welfare reform. Thus Japan shares many of the factors promoting the introduction of market mechanisms with other countries. However, Japan still lags behind in shifting to private care services (Figure 1).
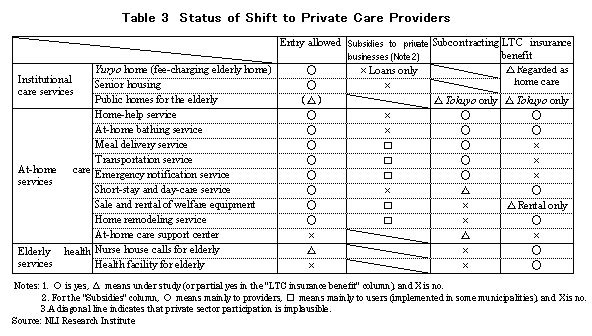
5. Impediments to Market Mechanisms in Japan One difference between the West and Japan in welfare administration is that while the West has little discrimination between public and private services, Japan clearly differentiates between public and private services in terms of entry barriers and subsidies. Specific restrictions on private services include: (1) absence of public funding (public services are funded by taxes, but private services are not eligible for subsidies), and (2) restricted entry (private companies are not allowed to operate public homes for the elderly). These restrictions impede the introduction of market mechanisms. Since at-home care services do not require licenses, there are no restrictions on private companies to provide these services. However, fair competition between public and private sectors is impeded by the existence of price differences since private companies cannot receive public subsidies. Private companies cannot even operate publicly funded institutional care services. Under Article 4 of the Social Welfare Service Law and Article 15 of the Law for the Welfare of the Aged the management of public homes for the elderly -including tokuyohomes (special nursing homes for the aged), yogohomes (nursing homes for the aged), and keihihomes (homes with moderate fee) -is restricted to municipalities and Shakai Fukushi Hojin(private companies cannot operate public homes for the elderly under present law). The only area relegated to private companies is the management of yuryohomes (fee-charging homes for the elderly). Still, they receive no public subsidies (excluding loans from the Social Welfare and Medical Service Corporation).
|
|
6. LTC Insurance Will Promote Shift to the Private Sector The LTC insurance to be implemented in April 2000 will propel the introduction of market mechanisms in long-term care services. It will put public and private sectors on an equal price footing, and competition will be fairer due to the shift from administered care to personal contracts. However, the extent of these effects will be limited. While LTC insurance will reduce the public-private disparity in public subsidies, it will not directly lead to eliminating entry barriers. Thus market mechanisms will be mostly limited to at-home care. To introduce market mechanisms in institutional care, entry restrictions will need to be eased to allow private companies to manage public homes for the elderly.
|

|
7. Requisites to Introducing Market Mechanisms In the West, the introduction of market mechanisms for long-term care services has led not only to increased efficiency, diversity, and flexibility of services, but to greater availability of alternative services. For example, the Community Care reform in the U.K. triggered the proliferation of short-stay and other services which had previously been uncommon, and also reduced delays in processing both complaints and requests. With the introduction of long-term care insurance in Germany, competition from small private providers has prompted the six huge bureaucratic welfare organizations to improve the quality and efficiency of services. However, allowing private providers into long-term care services has not been without problems. In the 1970s and 1980s, problems of inferior service quality (such as in nursing homes) frequently arose in the U.S. due to managements who zealously cut costs to increase profit margins. In addition, while a reliable and constant supply is needed for long-term care and other social services, opportunistic businesses selectively denied these services in a practice called "cream skimming"7-avoiding construction of nursing homes in low-income areas and turning away elderly patients who were poor. To alleviate these problems, legal and institutional measures were taken with the aim of controlling quality and protecting the rights of users, including the establishment of standards of service, third-party monitoring and complaint processing, and an ombudsman system. In Japan, although companies are refused entry ostensibly to assure quality (entry restrictions), there are hardly any adequate measures on the results side to ensure that quality control and protection of rights (exit restrictions). However, restricting entry to public and non-profit providers does not guarantee sound business rationale or high quality of service, as is apparent from frequent improprieties at social welfare corporations.8Before introducing market mechanisms into long-term care services, rather than restricting the types of service providers to try to assure quality, we first need to encourage a diverse variety of service providers and thereby assure users more choices. Once that occurs, we can develop systems to evaluate and monitor quality, and to resolve disputes and complaints.
|

|
Notes
References Go, Kazuhisa, "Competition Intensifies in Germany's Nursing-Care Services," Bamboo, November 1997. Komamaru, Kohei, "The Policy Research Framework for Introducing Market Mechanisms in Social Services in the U.K.," Kaigai Shakai Hosho Joho (Overseas Social Security Information), Fall 1995. Japan Small Business Corporation, "Status of Europe's Long-term Care Service Industry," a commissioned study by NLI Research Institute, 1997. Maruo, Naomi, "Social Welfare in Sweden After the ÄdelReforms," Shukan Shakai Hosho (Social Security Weekly), October 14, 1996. Le Grand, J. and W. Bartlett, "Quasi-Markets and Social Policy," Macmillan, 1993. OECD, "Caring for Frail Elderly People: Policies in Evolution," 1996.
|
Kazuhisa Go
Research field
レポート紹介
-
研究領域
-
経済
-
金融・為替
-
資産運用・資産形成
-
年金
-
社会保障制度
-
保険
-
不動産
-
経営・ビジネス
-
暮らし
-
ジェロントロジー(高齢社会総合研究)
-
医療・介護・健康・ヘルスケア
-
政策提言
-
-
注目テーマ・キーワード
-
統計・指標・重要イベント
-
媒体
- アクセスランキング